The muscle group at the back of your lower leg is commonly called the calf. The calf comprises of 2 major muscles called the gastrocnemius and soleus. Both of these muscles insert into the heel bone via the Achilles tendon. During contraction of the calf, tension is placed through the Achilles tendon. When there is too much repetitive force, the Achilles tendon can become inflamed and cause small micro tearing in the tendon. This inflammation and micro-tearing is termed Achilles tendinopathy.
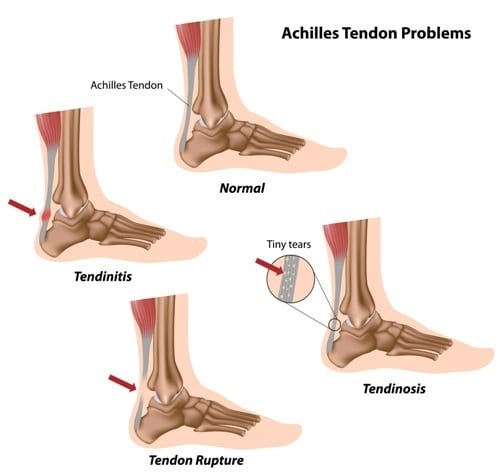
What are the symptoms of an Achilles Tendinopathy?
Symptoms may increase during activities which place strain on the Achilles tendon such as walking (especially uphill), going up and down stairs, running, jumping, hopping, or when performing heel raises or calf stretches. It is also common for patients to experience pain after these activities with rest. Symptoms may also be worse in the morning, for example walking in the morning after may be stiff and painful. Swelling in the Achilles region and pain on firmly touching the Achilles tendon are also common.
Patients with Achilles tendonitis or a degeneration of the Achilles may experience swelling, tenderness on firm touch to the Achilles tendon, weakness and palpable thickening of the affected Achilles tendon when compared to the unaffected side. They may experience noticeable stiffness and pain in the night or mornings especially after performing aggravating activities such as walking, hopping, jumping.
How can physiotherapy help?
A physiotherapist can massage the area to realign the tendon fibres whilst increasing blood flow to enhance the healing process. Rest is important in the early stages and our physiotherapists can provide support such as strapping or bracing. Furthermore, with healing progress the physiotherapist can advise on stretching & strengthening exercises. Further treatment options are also available such as acupuncture to promote natural healing of the tendon or mobilisation to encourage a return to mobility of the joint.
Acupuncture can also be significantly helpful with achilles tendinopathy, supplementing physiotherapy treatment. Acupuncture helps to reduce pain by activating your bodys’ natural pain reducing neural pathways, increase blood flow aiding your bodys’ natural healing process to the area and aid in the restoration of movement.
